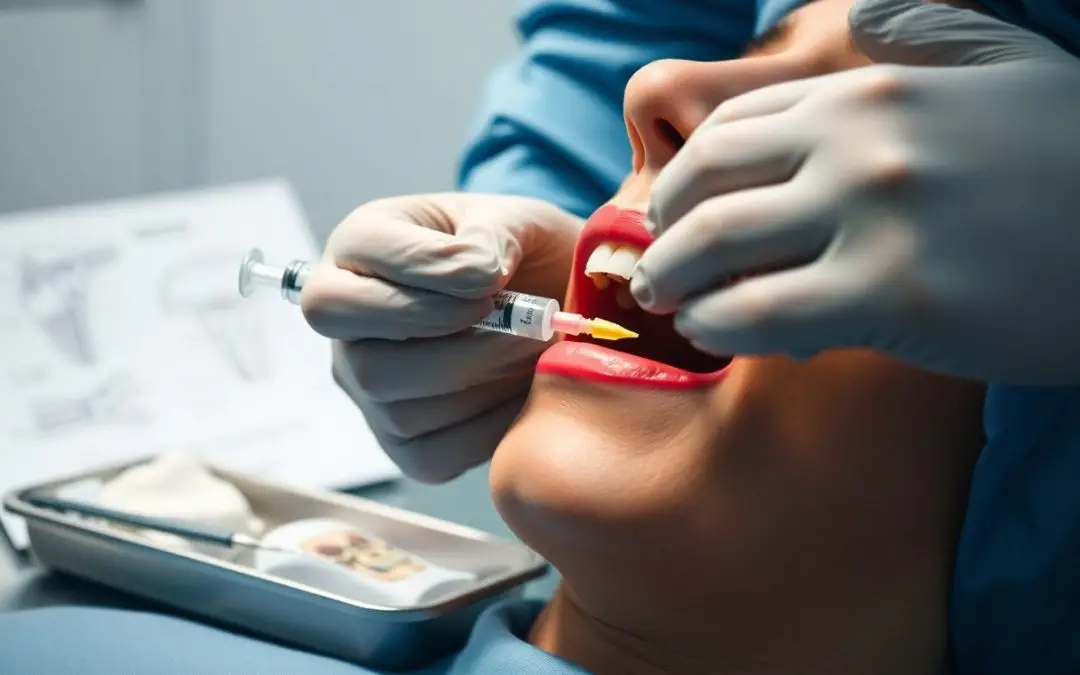
TMJ disorders can cause persistent jaw pain, headaches, and muscle tension that interfere with daily life. You may have heard about Botox as a treatment option and wonder if it truly works. This article explains how Botox affects jaw muscles, what research shows about its effectiveness, and whether it could be a safe choice for your TMJ symptoms.
The Ache in the Bone
Your jaw doesn’t just tense-it aches deep within the bone, a dull throb that radiates with every chew, yawn, or word. This isn’t fleeting discomfort; it’s a persistent signal from your temporomandibular joint that something’s out of alignment. Night after night, the pressure builds, turning simple motions into painful reminders.
The jaw is a hard place that clenches in the night.
While you sleep, your jaw tightens without warning, clamping down with force you’re unaware of until morning. This unconscious clenching strains the muscles and stresses the joint, setting the stage for daily discomfort. You wake with a tightness that feels locked in place, as if your face refuses to relax.
The teeth grind together and the hinge of the face becomes weary.
Grinding wears down enamel, but the damage goes beyond your teeth. The constant friction fatigues the joint and surrounding muscles, leaving your entire jaw system exhausted. Each grind adds strain to a hinge not built for relentless motion, weakening its function over time.
Chronic bruxism doesn’t just erode your teeth-it overwhelms the temporomandibular joint with repetitive stress that disrupts its natural mechanics. The joint’s disc can shift, inflammation sets in, and muscle tension becomes a constant companion. This cycle of wear and fatigue often leads to chronic pain, limited movement, and a face that feels permanently tense. Botox may help by calming the overactive muscles responsible for the grinding, offering relief where rest alone cannot reach.
The Medicine of the Needle
You’ve likely heard of Botox for smoothing wrinkles, but its role in treating TMJ pain runs deeper. When injected precisely into overworked jaw muscles, it acts like a reset button, quieting the constant tension that leads to headaches and discomfort. This isn’t cosmetic-it’s corrective.
The doctor uses a toxin to make the muscle go quiet.
A trained specialist administers small doses of botulinum toxin into your masseter or temporalis muscles. This substance temporarily interrupts the signals that cause excessive clenching. You won’t feel it during the procedure, but soon after, the persistent tightness begins to ease.
It blocks the nerve so the jaw can no longer fight the head.
Nerve signals that once triggered relentless jaw contractions are disrupted by the toxin. Without those commands, the muscle relaxes, breaking the cycle of strain between your jaw and skull. Relief often follows as pressure on the joint decreases.
Your jaw has been locked in a silent battle, tensing against your skull with force you weren’t aware of. When Botox blocks the nerve-muscle connection, it doesn’t paralyze-it recalibrates. The muscle can’t clench uncontrollably, giving the joint space to rest, inflammation a chance to fade, and your daily comfort a real improvement. This isn’t a permanent fix, but a strategic pause that allows healing to begin.
The Sting of the Treatment
You feel a brief pinch, nothing more-just a quick sting as the needle breaks the skin. This momentary discomfort targets the root of your jaw tension, aiming to quiet the constant clench. Relief often begins within days, making the fleeting sensation worthwhile.
You wait in the clean chair for the sting of the needle.
You sit still, jaw already aching from years of tension. The cool wipe of alcohol precedes the injection, then a sharp tap-you flinch, but it’s over in seconds. Each poke is precise, placed to relax the overworked muscles beneath your skin.
It is a small pain that takes away the larger one.
You endure a momentary jab to silence the daily throb behind your ears, the headaches, the grinding. That brief sting delivers relief most haven’t found elsewhere. The trade-off becomes clear quickly: seconds of discomfort for weeks of ease.
What makes this small pain worthwhile is how effectively it interrupts the cycle of muscle overactivity. Botox blocks nerve signals that cause excessive contractions, giving your jaw a chance to rest. You’re not masking pain-you’re resetting the system that’s been working too hard for too long.
The Softening of the Face
You may notice subtle changes within days of your Botox treatment. As the masseter muscles relax, the lower face begins to appear less rigid. This softening isn’t dramatic-it’s a gentle shift, like tension melting after a long-held breath. Your reflection starts to look more at ease, even at rest.
The tension leaves the face after the sun has risen seven times.
You wake up a week later and realize you haven’t clenched your jaw upon rising. That familiar tightness along your temples and jawline is gone. Your facial muscles feel lighter, as if a constant hum of strain has finally been switched off. Relief settles in quietly, almost unnoticed at first.
The square look of the jaw softens and the morning is better.
Your jawline appears less angular as the masseter muscles reduce in size. This change brings more balance to your facial contours. Mornings feel different-your head doesn’t ache, your teeth don’t throb. You start the day without the weight of tension dragging you down.
With repeated Botox treatments, the reduction in muscle bulk becomes more apparent, leading to a naturally softer jawline. This isn’t just cosmetic-small changes in muscle activity can significantly reduce joint stress and improve TMJ symptoms over time. You’re not only looking more relaxed, you’re functioning better, with fewer headaches and less fatigue in the face.
The Risk of the Crooked Smile
Some patients notice asymmetry in their smile after Botox for TMJ, especially if the injection spreads unevenly. You may feel self-conscious at first, but this typically resolves as the product wears off. Your provider’s technique plays a major role in minimizing this risk.
A bad needle can make the smile go crooked for a season.
Improper placement or a shaky hand during injection can weaken the wrong facial muscles. You might struggle with smiling naturally or feel like one side lifts less. This imbalance usually fades within weeks as Botox metabolizes.
The skin may turn blue for a time but the bone will rest.
Minor bruising at the injection site can leave a bluish tint under the skin. You’ll likely see it near the jawline where pressure builds. It’s temporary and doesn’t affect the treatment’s deeper benefit to your joint.
Bruising occurs when the needle nicks a small blood vessel during injection, leading to localized discoloration. You may notice tenderness or a dusky hue, but it typically clears in 7-10 days with no lasting harm. Applying gentle cold compresses can help reduce swelling and speed recovery, allowing you to focus on the relief Botox brings to your jaw tension.
Finding the Right Hands
Choosing the right provider for Botox treatment for TMJ pain shapes your entire experience. Your jaw’s complexity demands precision, so expertise matters more than cost. You need someone who sees beyond cosmetics and understands neuromuscular function. This isn’t just about injections-it’s about targeted relief.
Find a man who has studied the anatomy of the skull.
A provider’s knowledge of cranial structure determines treatment accuracy. You want someone who’s spent time learning how muscles, nerves, and joints interact in the jaw. This depth of understanding prevents complications and ensures Botox reaches the right points. Expertise in skull anatomy separates effective treatment from guesswork.
It is better to pay the price than to have the work done poorly.
Undergoing Botox for TMJ is an investment in comfort and function. A lower price might mean inexperienced hands or diluted technique. You risk asymmetry, ineffective results, or worsening tension. Paying more for a skilled specialist often saves you time, pain, and extra costs down the line.
Skimping on treatment can lead to prolonged discomfort or even structural imbalances in your bite and jaw movement. When Botox is placed incorrectly, it may weaken unintended muscles, altering how your jaw functions. A qualified specialist uses precise dosing and placement based on your unique symptoms. Yes, fees may be higher, but so is the likelihood of real, lasting relief. Your jaw works constantly-don’t compromise its care.

To wrap up
With these considerations, you understand that Botox may offer relief from TMJ pain and jaw tension by relaxing overactive muscles. While not a cure, it can be a helpful part of your treatment plan when used under professional guidance. Your results will vary based on individual factors, so discussing risks and benefits with your provider is necessary.